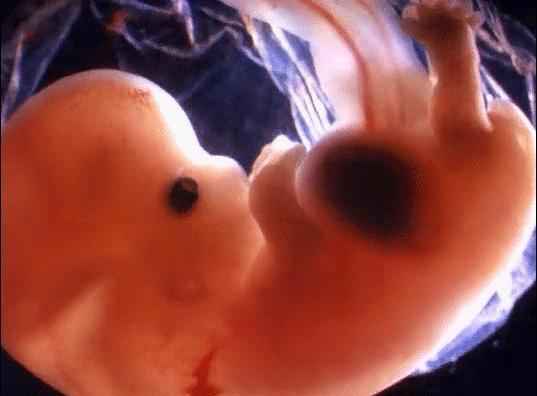
ARE YOU ENJOYING YOUR TIME IN THERE?
I would like to stay true to the description of this blog and take a trip down memory lane to share the steps that brought us here. For anyone considering how to approach lesbian fertility, our story may help you to make some critical decisions, or it may solidify ones that you are already planning on making. First, this book was one of our guides. The author weaves in her own story of conceiving her daughter and she shares some hilarious moments. The other essential text was Taking Charge of Your Fertility. It is a classic and the author has a helpful website: http://www.tcoyf.com/.
MY VERSION OF THE BIBLE
I am going to break our tale into its three stages: trying at home (dumb), going to a boutique-y fertility doctor (horrifying), and using a center for advanced reproductive services (BINGO!).
Trying at Home
All lesbian pregnancy scenarios begin with the big, looming question regarding the source of the sperm. Although we had two different friends volunteer to share theirs, we realized that the legal ramifications of this could be catastrophic. Even with professionally drawn documents, a known sperm donor can sue for rights to his "child." Remember, the cryobanks are going to do all of the important work for you by screening the donor, checking for STDs and genetic diseases, and working through your doctor to ship and deliver the units. We discovered that our closest reproductive health centers would need nearly a year to do this and they also would make us pay more than $1,000 to store the sperm. All of these indications pointed to using a cryobank and we did. There are a number of reputable ones, including California Cryobank, Fairfax Cryobank, and Xytex. They are expensive, so have a pregnancy fund before you begin.
Here are the at-home supplies one needs to do an ICI solo. Note- there is somewhere between a 0%-10% chance that it will work this way:
1. a headlamp- Use your imagination!
2. disposable speculums- No imagination needed!
3. a long, flexible catheter- That cervix is A LOT farther away than you think!
4. a microscope- Need to check that the sperm thaws properly!
5. WASTED TIME- THIS REALLY DOESN'T WORK VERY WELL AND YOU AND YOUR PARTNER WILL FEEL LIKE YOU DON'T KNOW WHAT THE HELL YOU ARE DOING.
We attempted the at-home method 4-5 times, alternating between the two of us. We thought it would offer a more comfortable setting and a feeling of home. It was just frustrating. I do know a couple who have two children by this method, but I get the sense that it rarely works. (They also used "fresh" sperm from a known donor.) I would avoid it, but that is just my opinion. Keep in mind that I don't do well when I have to go to the dentist. This really was not for me or for most people.
Going to a Fertility Doctor
Next, we decided to see a fertility doctor to pursue IUI. What we did not necessarily realize was that he was more of an OB/GYN who was willing to address our fertility needs. He was not an endocrinologist. He was approximately 70 years old. We still did not want to feel like we were on a fertility assembly line at one of the big reproductive health offices. He suggested that we try a different sperm donor. We did that. He also monitored each of us a little more closely. He did have a "fertility hotline," but we used an at-home ovulation prediction kit to known if it was time for the IUI. I think I had blook work once or twice with him. His hands shook.
He was the only physician in his office who performed reproductive services of this nature, so we need to see an "on call" doctor at the hospital, if we required an IUI on a weekend. At one point, he suggested I try clomid for two cycles. It made me feel like I was suffering in purgatory. He was clumsy and, in retrospect, did not have the means to track us enough to achieve a positive pregnancy. After 8 or more attempts with him, we moved on. It was sort of like we were stuck in the middle of a long staircase. I know that he helped some couples get preganant, but my hunch is that this was just due to good luck.
STUCK ON THE IUI STAIRCASE

Using a Center for Advanced Reproductive Services
At this point, I felt I was too old to continue with the process. Tommie, at 2.5 years younger, seemed like the better candidate. Plus, she was willing to face IVF. Based on recommendations from close friends who have a daughter and another on the way, we chose our fertility doctor at The Center. We LOVE him. The Center requires that you attend an IVF seminar before you begin the process. We did that. They also force you to see a psychologist to discuss the ramifications of using a sperm donor. We did that too, but it was a waste of time and money. The woman was condescending and we both wanted to strangle her when she asked, "Is there any history of abuse at home?" and "Do either of you have any mental health issues?" We wondered why straight couples, using their own sperm and egg, are not required to sit through this insulting process. We reminded ourselves of the goal: a baby.
Tommie and I then met with our doctor. He put her through a battery of tests and she passed with flying colors. Then, we began the injections, the sickness from the injections, the retrieval surgery, and two transfers. The second one was successful and now we have Sharkie. It was not fun, but we currently have the result we wanted. In addition to the side effects of the injections, we had to travel to The Center (40 minutes away) on a daily basis, for weeks at a time. We also only saw our own doctor once. When you work with a group that large, they all share the duties. Tommie's successful second transfer was performed by a doctor we had never even met before that day. Indeed, it felt like the assembly line we anticipated. We would see the same people in the waiting room every day. We watched them cycle through, some with smiles and others with tears. We sometimes waited for an hour or more to see the doctor. We passed our time watching the TV that cut in and out of service. We saw people we knew and we actually made new friends. We will go for our second ultrasound on Friday. If Sharkie is doing well, we will be "dismissed" to go to an OB/GYN of our choice. It has been approximately five years since we began our journey.
Using a comprehensive reproductive health center was our last choice, but we think it was the best one. They did all of the work for us. They charted Tommie's ovulation. They were always open for tests and procedures. They provided statistics to show that nearly 65% of women in Tommie's age group conceive through them. They had their own embryologists. When our first transfer did not succeed, they had the answers as to why. They stored the sperm and the emryos. The best part was that almost every bit of it was covered under our health insurance. It was a relief to go there.
No comments:
Post a Comment